Holistic Support for High-Risk HPV Infection
Personalised Cervical Health Care with Expert Gynaecological Review
Personalised Cervical Care Guided by Specialist Gynaecologists
Receiving a high-risk HPV (HR HPV) result can feel overwhelming. You may have been told your cytology is normal, or perhaps you’ve been discharged from colposcopy but still feel uncertain about what comes next.
At Your Health, we provide personalised, evidence-based support for women with persistent high-risk HPV infection.
Our approach combines Consultant Gynaecologist review, clinical oversight, and supportive therapies including Papilocare®, helping you take proactive steps toward restoring and protecting your cervical health.
You are not alone — and there is a structured, supportive pathway forward.

Key Information to Help You Feel Informed
Human papillomavirus (HPV) is one of the most common viruses worldwide. There are over 200 types, with around 40 affecting the genital area.
Most sexually active people will be exposed to HPV at some point in their lives.
HPV types fall into two main categories:
- Low-risk HPV – may cause genital warts but does not cause cancer
- High-risk HPV (HR HPV) – can cause cellular changes that may lead to cancer if infection persists
High-risk HPV refers to specific strains that can damage cervical cells over time.
The most significant types are:
- HPV 16
- HPV 18
Together, these two strains account for approximately 70% of cervical cancers worldwide.
Other high-risk types include:
31, 33, 45, 52 and 58.
It is important to remember:
Most high-risk HPV infections clear naturally. The concern arises only when the virus persists over time.
High-risk HPV is transmitted through skin-to-skin sexual contact, not just intercourse.
Transmission can occur through:
- Vaginal sex
- Anal sex
- Oral sex
- Close genital skin contact
Important facts:
- Condoms reduce risk but do not eliminate it
- HPV can be present without symptoms
- You may carry HPV for years without knowing
High-risk HPV infection is extremely common:
- Most sexually active individuals will contract HPV at least once
- In around 90% of cases, the immune system clears the virus naturally within 1–2 years
- Only a small percentage develop persistent infection
If your body hasn’t yet cleared the virus, this does not mean you have done anything wrong. It simply means your immune system may need additional support.
Why Does Persistent HPV Matter?
High-risk HPV only becomes dangerous if it remains in the body.
If persistent, it may:
- Cause abnormal cell changes
- Lead to precancerous cervical lesions
- Progress slowly (often over 10–20 years) toward cancer if untreated
This long timeframe means there is opportunity to intervene, support healing, and monitor safely.
A Personalised, Holistic Approach with Your Health
At Your Health, we specialise in supporting women who:
- Have tested positive for high-risk HPV
- Have negative cytology (no abnormal cells)
- Have had abnormal cytology but completed colposcopy treatment
- Have been discharged from NHS colposcopy services
- Want proactive cervical health support
Our care pathway begins with a Consultant Gynaecologist review of your cervical smear and screening results, ensuring your treatment plan is medically appropriate and individually tailored.
We combine:
✔ Specialist clinical oversight
✔ Holistic cervical support
✔ Evidence-based therapies
✔ Ongoing monitoring and reassurance
Papilocare® – Clinically Studied Cervical Support
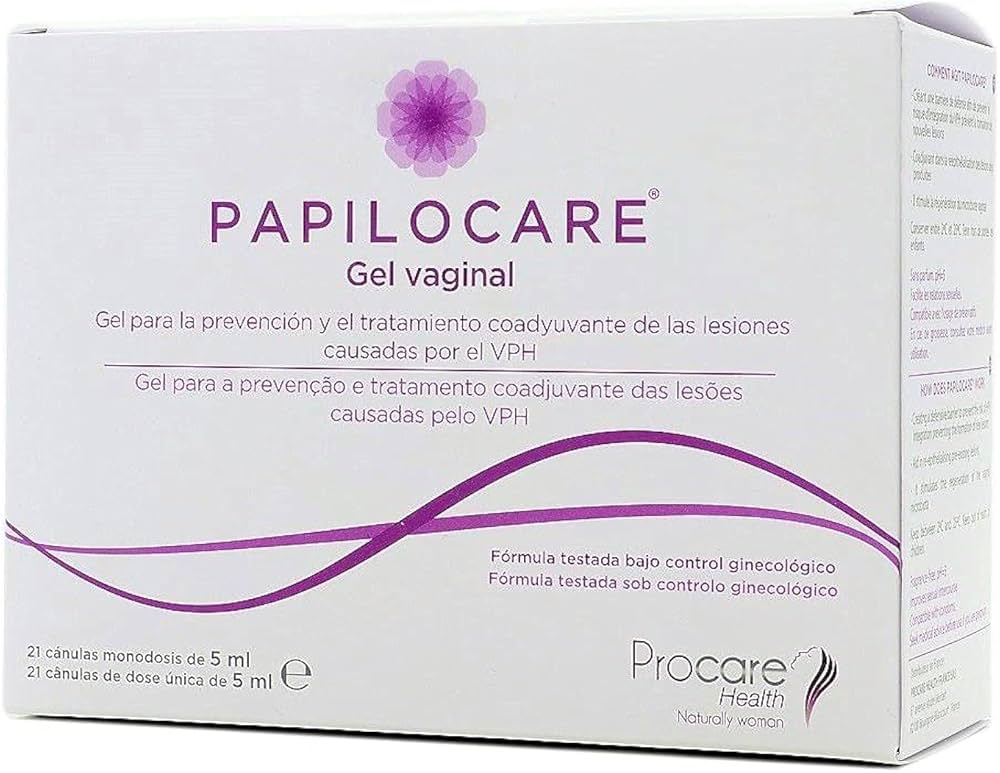
Papilocare® vaginal gel is a clinically studied, non-hormonal therapy designed to support cervical healing in women with HPV infection.
It is suitable for women over 18 who:
- Have started sexual activity
- Have confirmed HPV infection
- Have been reviewed by a healthcare professional
Papilocare® works to:
- Re-epithelialise the cervical transformation zone
- Support normalisation of low-grade intraepithelial lesions
- Restore vaginal microbiota balance
- Improve cervico-vaginal mucosal integrity
- Reduce vaginal dryness
- Promote overall cervical and vaginal health
Clinical studies suggest many women experience improvement in cervical lesions and achieve negative high-risk HPV tests within months, without significant side effects.
Your Personalised HPV Care Pathway
Step 1 – Secure Online Clinical History
Complete your confidential online medical proforma and upload your latest cervical smear results.
Step 2 – Consultant Gynaecologist Review (Within 48 Hours)
Your results are reviewed by our specialist, who confirms suitability and creates a personalised care plan.
Step 3 – Tailored Treatment Plan
This may include:
- A 6-month Papilocare® vaginal gel course
- Standard or intensive regime (depending on clinical history)
Step 4 – Treatment Delivered to Your Door
Your therapy can be delivered securely in full or in staged supply, allowing you to begin treatment from the comfort of home.
Step 5 – Ongoing Monitoring & Support
We guide you through:
- Ongoing clinical support and reassurance
- HPV re-testing
Treatment Programme Overview
A typical Papilocare® course involves:
- Month 1: 21 applications
- Months 2–6: 11 applications per month
Two regimes are available:
- Standard (as above)
- Intensive (3 months daily, then 3 months alternate days)
Your exact plan is determined following specialist review.
Investment in Your Cervical Health
Our full structured pathway includes:
- Administrative and support services
- Initial triage and specialist review
- Full 6-month Papilocare® course
- Clinical oversight
- Ongoing monitoring
Total programme investment: £850.00
This includes product supply, clinical assessment, delivery and personalised oversight.
Our Specialists

Mr Fateh Ghazal
Consultant Gynaecologist, Diploma of Advanced Endoscopy
Mr F Ghazal has over 10 years of experience as consultant Gynaecologist with special interest in minimal access surgery, oncology, colposcopy and management of vulval disease. He has his Diploma of advanced endoscopy from Surrey University and obtained extensive specialised training in minimal invasive surgery.
He is an accredited colposcopist and is experienced in managing women with vulval disease in addition to general gynaecology conditions including endometriosis and adenomyosis. He has an excellent track record of providing the highest quality of care with exceptional patient satisfaction.
His area of interest are Laparoscopic surgery (keyhole) for hysterectomy, ovarian cystectomy, removal of ovaries, fallopian tube surgeries, treatment of endometriosis, Laparotomy including hysterectomy and complex gynaecology surgeries, Hysteroscopy surgery including vaginoscopy, Colposcopy, loop treatment of cervix, treatment of vaginal precancer conditions, vulvoscopy and vulval surgery.

Prof Tony Thomas
Consultant Gynaecologist Specialist in Gynaecological Surgery
Professor Tony Thomas is a distinguished consultant gynaecologist with over 25 years of dedicated service to improving women’s health and well-being.
Collaborating with his esteemed colleagues, Prof. Thomas brings extensive expertise in managing a wide range of gynaecological conditions, always prioritising compassionate, patient-centred care.
With a strong background in keyhole gynaecological surgery, Prof. Thomas is a trusted leader in his field. He heads the gynaecological cancer service at this trust and possesses extensive experience in managing menopause-related concerns.
A recognised authority in the diagnosis and treatment of pelvic pain, Prof. Thomas understands the lengthy, costly, and often frustrating journey many women face in seeking a diagnosis. To address this, he has collaborated with like-minded colleagues to enhance the availability of the Endosure test, a 30-Minute Clinical Decision Support Tool which has relatively recently been made available in the United Kingdom. This innovative, non-invasive diagnostic tool could facilitate the early identification of endometriosis, a common cause of pelvic pain. By reducing the reliance on diagnostic laparoscopy, Endosure offers patients a quicker, less invasive, and more cost-effective preliminary evaluation option.
In addition to his diagnostic expertise, Prof. Thomas maintains a high surgical workload in keyhole procedures. His extensive surgical experience ensures that patients can confidently entrust their care to him should further surgical evaluation or intervention be required.
Prof. Thomas remains committed to advancing women’s health through cutting-edge treatments and improved diagnostic pathways, ensuring every patient receives the highest standard of care.including hysterectomy and complex gynaecology surgeries, Hysteroscopy surgery including vaginoscopy, Colposcopy, loop treatment of cervix, treatment of vaginal precancer conditions, vulvoscopy and vulval surgery.

Dr Lina Antoun
Consultant Gynaecologist, Specialist in Pelvic Pain & Endometriosis
Dr. Lina Antoun is a highly experienced Consultant Gynaecologist with a special interest in pelvic pain and endometriosis. She is dedicated to providing compassionate, evidence-based care for women experiencing complex gynaecological conditions.
Alongside her clinical practice, Dr. Antoun is actively involved in pelvic pain and endometriosis research, ensuring her patients benefit from the latest advances in diagnosis and treatment. Her work bridges the gap between cutting-edge research and patient-focused care, with the aim of improving outcomes and quality of life for women.
Areas of Expertise
- Endometriosis diagnosis and management
- Chronic pelvic pain treatment
- Minimally invasive (laparoscopic) surgery
- Menstrual disorders
- Reproductive health and fertility-related concerns
Research & Academic Work
Dr. Antoun plays an active role in clinical research projects exploring new ways to better understand and treat pelvic pain and endometriosis. Her research interests include:
- Improving early diagnosis of endometriosis
- Exploring advanced surgical and non-surgical management options
- Enhancing long-term care pathways for women with chronic pelvic pain
She frequently contributes to academic publications, international conferences, and collaborations with multidisciplinary teams, ensuring her work drives progress in women’s health.
Patient-Centred Approach
Dr. Antoun believes in listening first. She recognises that pelvic pain and endometriosis are complex, often misunderstood conditions, and takes time to fully explore each patient’s concerns. Her approach combines clinical expertise, empathy, and individualised care, empowering women to make informed decisions about their health.
Why Choose Your Health for High-Risk HPV Support?
✔ Consultant-led gynaecological review
✔ Evidence-based cervical support therapies
✔ Personalised treatment planning
✔ Holistic, immune-supportive approach
✔ Discreet home delivery
✔ Continued monitoring and peace of mind
We empower women to take informed, proactive control of their cervical health — with clarity, reassurance and specialist guidance.
Take the Next Step Toward Cervical Health
If you have tested positive for high-risk HPV and want structured, supportive care beyond “wait and see,” we are here to help.
Complete your confidential clinical history today and receive specialist review within 48 hours.
You deserve clarity.
You deserve support.
You deserve a proactive plan.
Book Today
Have Questions?
Get in touch – Our friendly team is here to support you every step of the way
